Can You Flush a Catheter With Normal Saline? Medical Protocol
Did you know that maintaining catheter patency and preventing complications is a critical aspect of patient care? Flushing a catheter with normal saline is a common practice, but understanding when and how to do it correctly can make a significant difference in outcomes. This introduction explores the medical protocols surrounding catheter flushing with normal saline, shedding light on its safety, purpose, and best practices. Whether you are a healthcare professional seeking to reinforce yoru knowledge or a patient curious about the procedure, this guide aims to clarify why normal saline is frequently enough preferred and how proper flushing supports catheter function and reduces infection risks. Keep reading to uncover essential insights that can enhance both care quality and patient comfort.
Understanding Catheter Flushing Basics With Normal Saline

Normal saline has become a cornerstone in catheter maintenance due to its simplicity,compatibility,and safety profile. Its isotonic nature means it closely mimics the body’s own fluids, which substantially reduces irritation or damage to the delicate internal lining of catheters and surrounding tissues.This makes it an ideal flushing solution to help maintain catheter patency and prevent blockages caused by clot formation or residual medication buildup.
Using normal saline for flushing isn’t just about keeping the catheter clear-it also plays a critical role in infection prevention and extending the device’s usable life.By routinely flushing with saline, healthcare providers can ensure that debris and stagnant fluids are effectively cleared, minimizing the risk of bacterial colonization. In practice, this frequently enough involves gently pushing pre-measured amounts of sterile 0.9% sodium chloride through the catheter at regular intervals or after medication administration.
- Simple and safe: Normal saline is non-irritating and can be used across most catheter types, including Foley catheters and central venous lines.
- Widely accessible: It is inexpensive and readily available in sterile, pre-filled syringes, which helps maintain sterility during flushing procedures.
- Compatibility: Normal saline is compatible with numerous medications and catheter materials, reducing the risk of adverse chemical reactions.
One practical tip to keep in mind: always use a gentle, steady pressure rather than forceful flushing. This prevents damage to the catheter lumen and surrounding tissues while ensuring effective clearance. Flushing with normal saline is often the first step before resorting to other solutions like heparin, especially for preventing clot formation in central catheters.By understanding the basic benefits and proper techniques of saline flushing, both clinicians and caregivers can confidently maintain catheter function and patient comfort without unnecessary complications[[1]](https://www.backtable.com/shows/urology/articles/how-to-flush-a-foley-catheter)[[3]](https://healthsystem.osumc.edu/pteduc/docs/FlushingCath.pdf).
Medical Protocols for Flushing Different types of Catheters

proper flushing protocols vary depending on the type of catheter in use, as the anatomical location, purpose, and material of catheters influence how and when saline flushing should be performed. Healthcare providers must tailor procedures accordingly to maximize catheter longevity, prevent complications, and ensure patient safety.
For urinary catheters, such as Foley catheters, flushing is typically done to clear blockages caused by sediment, blood clots, or mucus. Normal saline is favored for gentle irrigation because it is isotonic and non-irritating to the bladder lining. Protocols often recommend using sterile 0.9% saline in volumes ranging from 10 to 30 mL,delivered slowly via a catheter-tip syringe or irrigation set. The frequency depends on clinical signs like hematuria or catheter malfunction, but routine flushing every 4-6 hours may be advised in some settings to maintain patency without introducing infection risk[1].In contrast, central venous catheters (CVCs) require a more cautious approach. Flushing with normal saline is routinely performed before and after medication administration to prevent occlusion by thrombus or drug precipitates. Standard practice involves using 5 to 10 mL of sterile saline with a gentle, steady push to avoid catheter damage. For some types, like peripherally inserted central catheters (PICCs) and ports, protocols may include heparinized saline flushes after a normal saline flush to extend catheter patency further; though, normal saline alone has become more widely favored due to fewer complications and ease of use. Always adhere to facility-specific guidelines, as the flushing volume and frequency can depend on catheter lumen size and the patient’s coagulation riskspecific material properties influencing flushing technique. Softer materials may be more susceptible to damage from rapid or forceful flushing, so a slow, steady saline push is critical. Clinical teams should also be cautious when flushing lumens used for blood draws or those exposed to irritant medications to prevent precipitation or occlusion.
In all cases, adherence to institutional guidelines and reinforcing sterile technique during each flush remains paramount. Using pre-filled sterile saline syringes reduces the risk of contamination. Combining these protocols with careful observation for resistance during flushing or patient discomfort ensures timely intervention and helps maintain catheter patency effectively[1]Step-by-Step Guide to Safely Flush a catheter Using Saline flushing a catheter with normal saline is a crucial skill that, when done correctly, can maintain catheter patency and prevent complications like blockages or infections. The process requires precision,sterility,and gentle technique to avoid damaging the catheter or causing patient discomfort. Whether dealing with a urinary Foley catheter or a central venous line, following a consistent, stepwise method enhances safety and effectiveness. Begin by gathering all necessary supplies: sterile normal saline (0.9%), a catheter-tip syringe (often 10-60 mL depending on catheter type), alcohol swabs or antiseptic wipes, gloves, and a sterile field or surface. Hand hygiene is essential before donning sterile gloves to maintain asepsis. If flushing a Foley catheter, position the patient comfortably and place absorbent towels or a basin to catch any drainage. For vascular catheters, ensure the patient is in a stable position to reduce movement during the procedure. Many practitioners find it helpful to pre-fill syringes with sterile saline prior to the procedure to avoid contamination and minimize time spent manipulating connections.Using a catheter-tip syringe (designed for optimal fit) ensures a safer, leak-free flush. For example, Foley catheters typically require 10-30 mL of saline flushed gently every 4-6 hours or as signs dictate, while central venous catheters use smaller volumes (5-10 mL) with each medication administration or routine maintenance. Avoid rapid or forceful flushing, which can dislodge thrombi or damage soft catheter materials such as silicone. If resistance is felt, never push harder; rather, pause, re-assess, and seek guidance if necessary. Also, always prioritize sterility-failure to maintain aseptic technique during flushing can introduce pathogens and precipitate bloodstream or urinary tract infections. by mastering these detailed steps, healthcare providers can confidently manage catheter care, improving patient outcomes and reducing catheter-related complications. This approach blends clinical precision with practical care, highlighting the importance of technique and vigilance during saline flushing procedures. Another common pitfall lies in breaching sterility, which can turn a routine flush into a source of infection. It’s tempting to forgo the full aseptic preparation when in a hurry, yet failing to properly disinfect ports or touching sterile syringe tips contaminates the system and elevates the risk of bloodstream or urinary tract infections. Always prioritize hand hygiene, use antiseptic swabs for at least 15 seconds on the connection sites, and avoid any contact with sterile parts. Maintaining a closed system as much as possible safeguards against introducing harmful pathogens. Additionally, improper assessment before flushing is a mistake that can compromise patient safety. Never flush if resistance is encountered or if signs of infection such as swelling, redness, or unusual discharge are present without prior evaluation. Forcing saline under pressure might worsen partial occlusions or push infectious material deeper into tissues. Rather, pause, reassess the situation, and consult healthcare guidelines or specialists if blockage or infection is suspected. Awareness of these warning signs helps prevent avoidable complications and guides appropriate intervention. by steering clear of these errors, clinicians and caregivers can enhance the safety and effectiveness of catheter flushing with normal saline, preserving catheter function and patient well-being.Preparation and Assembly
Step-by-Step Procedure
Practical Tips and Common Questions
Common Mistakes to Avoid When Flushing Catheters
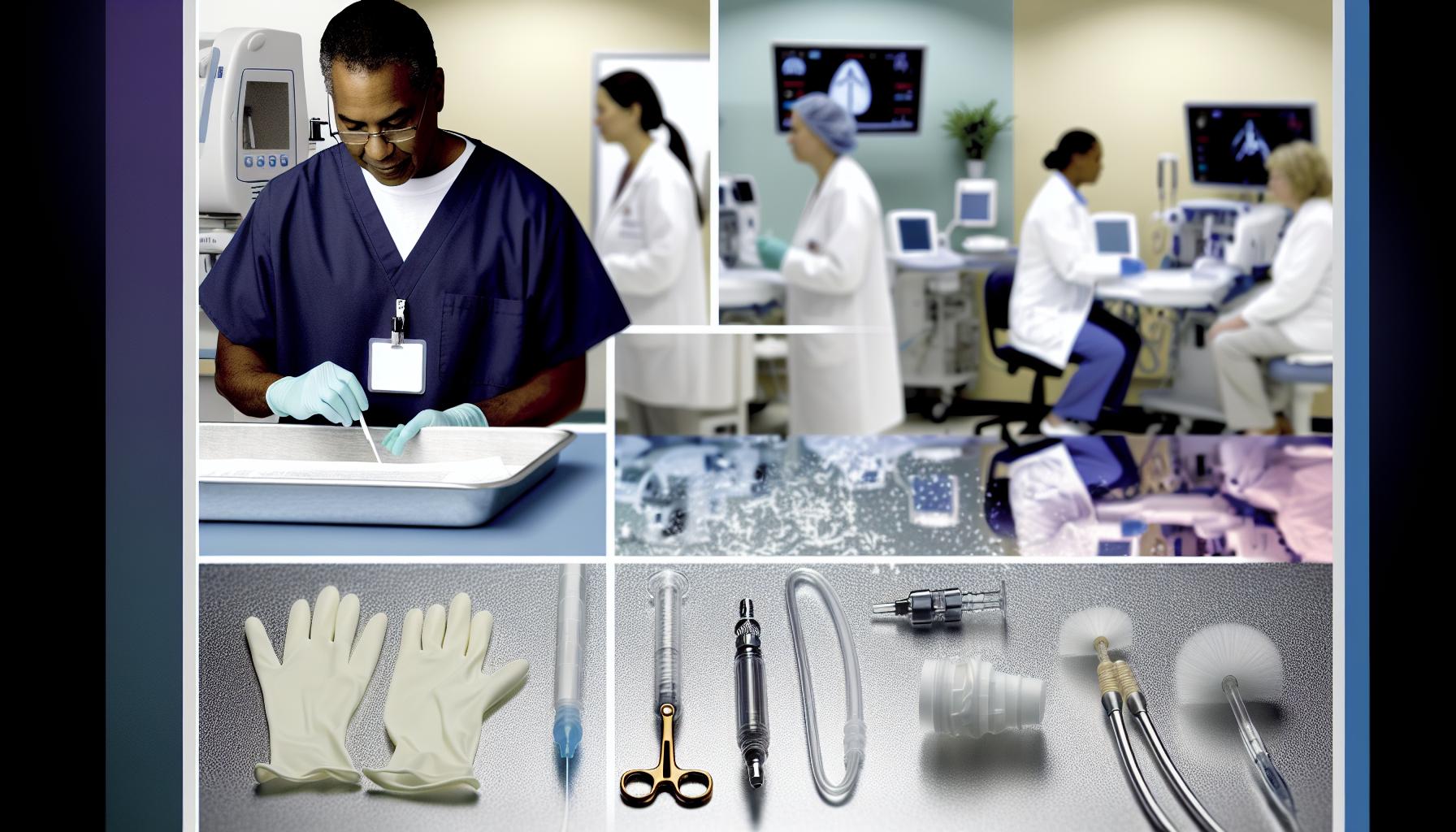
A surprisingly frequent error during catheter flushing is underestimating the importance of gentle technique. Many assume that flushing quickly and forcefully will clear blockages faster,but in reality,this can cause microscopic damage to delicate catheter materials and potentially dislodge thrombi or debris,leading to more serious complications. For example, in central venous catheters, excessive pressure may result in vessel injury or catheter rupture. Always remember that slow, steady flushing is not only safer but more effective in maintaining catheter integrity and patient comfort.Comparing Normal Saline to Other Flushing Solutions
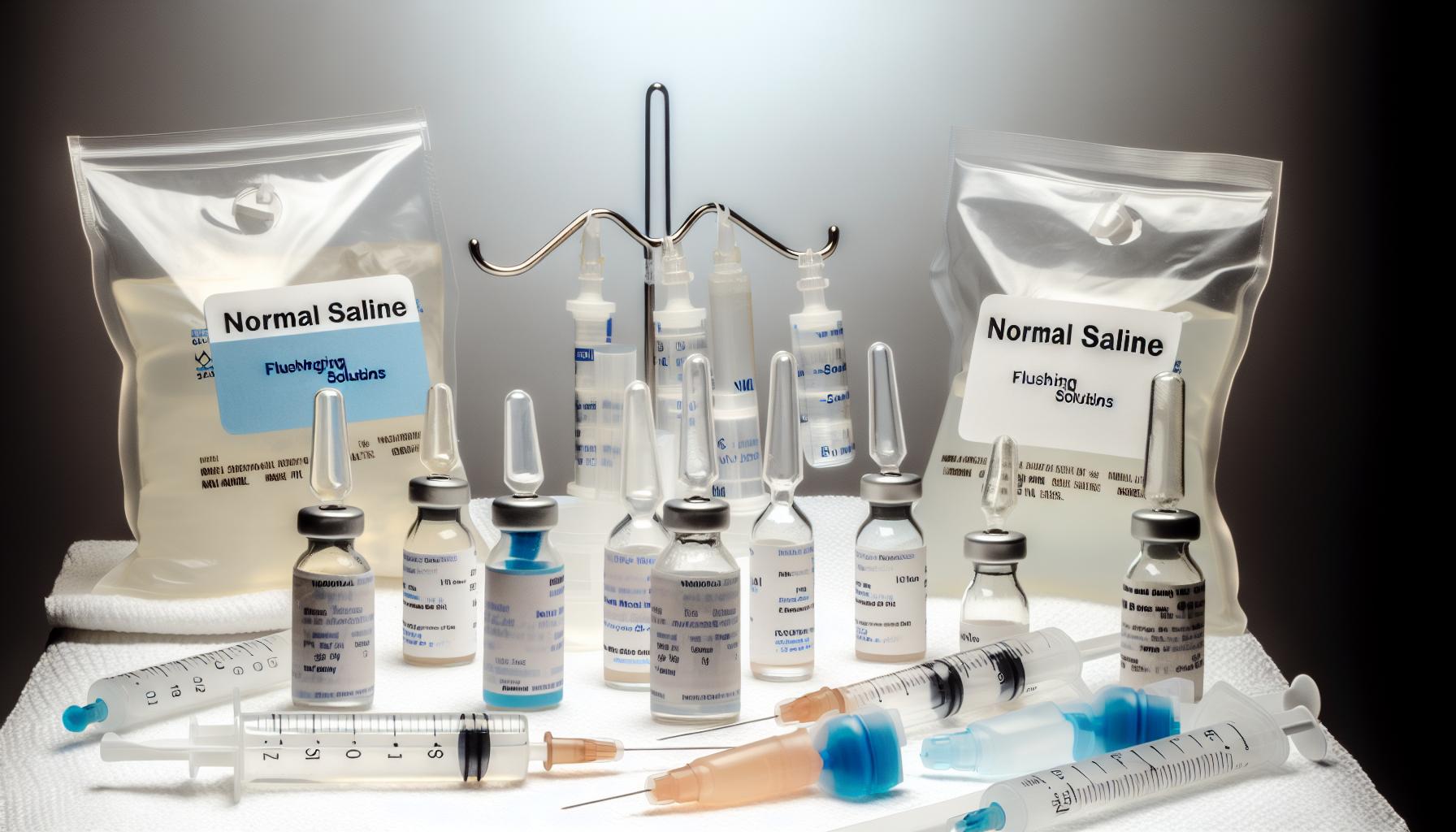
Flush solutions play a crucial role in maintaining catheter patency, and choosing the right one impacts both safety and effectiveness. Normal saline (0.9% sodium chloride) stands out as a non-anticoagulant, isotonic option widely favored for its simplicity and compatibility with most catheter types. However, when compared to alternatives like heparinized saline or acidic solutions, the decision often hinges on the catheter’s clinical context and specific risks involved.Heparin flush solutions have traditionally been used, especially in central venous catheters, to prevent thrombus formation by inhibiting clot advancement within the lumen. While effective for clot prevention, heparin introduces potential risks such as bleeding complications and heparin-induced thrombocytopenia. Moreover, recent studies suggest that normal saline flushes can be equally effective in maintaining catheter patency in many cases, reducing the need for anticoagulation. This has led to shifts in practice, especially in settings where the bleeding risk is significant or where there is concern about unnecessary anticoagulant exposure [[2]](https://aacnjournals.org/ccnonline/article-abstract/32/1/e12/4479), [[3]](https://ascopubs.org/doi/10.1200/JCO.2019.37.15_suppl.6501).Acidic washouts (e.g., citrate or acidic solutions) serve a different purpose, functioning mainly to dissolve mineral deposits or prevent encrustation in catheters, especially urinary catheters. These solutions are not typically used for routine flushing but can be valuable in specialized circumstances where saline or heparin fails to prevent blockages or when mineral scaling is a known problem. However, these carry a higher risk of irritation and potential damage to catheter material if overused or improperly applied [[1]](https://www.emjreviews.com/urology/news/exploring-saline-and-acidic-washouts-in-catheter-care/).Deciding Between Normal Saline and Other Flush Solutions
| Flush Solution | Primary Use | Advantages | Considerations |
|---|---|---|---|
| Normal Saline (0.9% NaCl) | General flushing,routine maintenance | Safe,isotonic,inexpensive,broadly compatible | Does not prevent thrombosis; might potentially be less effective in high-risk catheters |
| Heparinized Saline | Prevention of thrombus in central venous catheters | Effective anticoagulant properties | Risk of bleeding,allergies,requires careful dosing |
| Acidic Solutions (e.g., citrate) | Prevention/dissolution of mineral deposits | Useful for encrustation management | Can irritate tissue; may degrade catheter materials if misused |
ultimately, the choice of flushing solution should be tailored to patient needs, type of catheter, and clinical circumstances. For many patients, especially those with standard catheters and low clot risk, normal saline provides a reliable, safe, and cost-effective flush solution. Those managing central lines or specialized catheters must weigh the benefits of heparin or other agents in preventing thrombosis against their inherent risks.Consulting current evidence and institutional protocols will help ensure optimal catheter care and longevity.
Benefits and Risks of flushing Catheters With Saline

Flushing catheters with normal saline remains one of the most straightforward and widely endorsed techniques in clinical practice to preserve catheter function and prevent occlusions. One of the key advantages is its biocompatibility; as an isotonic solution, normal saline minimizes irritation to blood vessels and surrounding tissues, making it suitable for regular flushing across various catheter types without the risk of chemical damage or adverse tissue reactions. This gentle but effective approach helps clear residual medications and blood from the catheter lumen, reducing the risk of blockage due to clot or debris buildup.
Another notable benefit is saline’s safety profile. Unlike heparin-a commonly used anticoagulant flush-normal saline carries no risk of bleeding complications, allergic reactions, or heparin-induced thrombocytopenia. This makes it an invaluable alternative for patients who have contraindications to anticoagulants, such as those with bleeding disorders or those receiving surgery. Additionally, saline is cost-effective, readily available, and requires no special storage conditions, making its use practical and accessible in virtually all healthcare settings.
However, while saline performs excellently in routine catheter maintenance, it’s vital to understand its limitations. Normal saline does not possess anticoagulant properties, so in patients with higher thrombotic risks-such as those with long-term central venous catheters-saline alone may not fully prevent clot formation inside the catheter lumen. In such cases, supplementary use of heparin or other anticoagulants may be necessary, depending on clinical protocols and patient-specific risk profiles.
- Benefits of Normal Saline Flushing:
- Non-irritating isotonic solution safe for blood vessels and tissue
- Minimal risk of adverse reactions or complications
- Cost-effective and convenient for routine use
- Widely compatible across different catheter materials and types
- Risks and Limitations:
- Does not prevent clot formation in high-risk patients
- May require more frequent flushing intervals compared to heparin
- Not suitable for dissolving mineral deposits or encrustations
- Poor effectiveness if the catheter is already partially obstructed
For example, in urinary catheters prone to encrustation or catheter-associated infections, saline flushing alone might potentially be insufficient, necessitating acidic or antimicrobial flushes as adjunctive treatments [[1]](https://mft.nhs.uk/app/uploads/2021/05/Flushing-of-an-Indwelling-Catheter-and-Bladder-Washouts-Knowbots.pdf).Conversely, for peripheral or midline catheters used intermittently, saline flushes provide a simple yet effective maintenance routine, reducing the risk of harm linked to anticoagulants or complex flush protocols.
normal saline flushes offer a balance of safety, simplicity, and effectiveness ideal for routine catheter care.Clinicians and caregivers should evaluate patient-specific factors-such as bleeding risk, catheter type, and history of occlusions-to decide when saline is the best choice and when to consider alternative or additional flushing agents. This careful approach maximizes catheter longevity while minimizing avoidable complications.
When Not to Flush a Catheter with Normal Saline

It’s a common misconception that normal saline is universally appropriate for flushing all catheters in every clinical situation. While it’s generally safe and effective for routine maintenance, there are important scenarios where flushing a catheter with normal saline may be inadequate or even potentially harmful.Recognizing these circumstances is critical in tailoring catheter care to individual patient needs and avoiding unnecessary complications.
For patients with long-term or central venous catheters who are at high risk of thrombotic occlusions, saline alone may fall short. Since normal saline lacks anticoagulant properties,it does not actively prevent clot formation inside the catheter lumen.In such cases, relying solely on saline flushing might allow fibrin buildup or thrombus development, leading to catheter blockage or the need for replacement.Medical protocols frequently enough recommend using heparin flushes or other anticoagulant-containing solutions alongside or in place of saline for these high-risk catheters to maintain patency effectively.Therefore, using saline exclusively without anticoagulant supplementation could result in suboptimal catheter function and increased patient morbidity.
In addition, normal saline is ineffective for clearing encrustations or mineral deposits, a common problem particularly with urinary catheters. These catheter types can become obstructed by crystalline buildup related to urine composition or infection. Flushing with saline in such cases will not dissolve or remove these deposits and may delay more definitive treatment. Alternative solutions - such as acidic bladder irrigants or specialized antimicrobial flushes – are preferred to manage or prevent catheter encrustation and infection. this distinction underscores the importance of assessing catheter type and clinical indications before selecting a flushing agent.
Saline flushing is also inappropriate when a catheter is suspected to be mechanically occluded or partially blocked. If resistance is encountered during flushing or if urine output is consistently poor, forcing saline through a clogged catheter can cause damage or dislodgement and worsen complications. In these scenarios, clinicians must evaluate the cause of blockage thoroughly-such as kinking, clot formation, or biofilm accumulation-and may need to employ specific treatments like enzymatic thrombolytics or catheter replacement rather than simply flushing with saline.
- Situations Where Normal Saline Should NOT Be used alone:
- Long-term central venous catheters at high risk of thrombosis without anticoagulant support
- Urinary catheters with encrustation or mineral deposits
- catheters suspected of mechanical blockage or partial occlusion
- patients with ongoing catheter-associated infections requiring antimicrobial flushes
Ultimately,the decision to forego normal saline flushing should be informed by patient-specific factors such as catheter type,duration of use,clinical signs of blockage or infection,and institutional guidelines. Collaborating with healthcare providers to select appropriate flushing protocols ensures optimal catheter care and reduces risks associated with inappropriate flushing practices. Keeping these exceptions in mind empowers both clinicians and caregivers to maintain catheter function safely and effectively.
How Catheter Material Affects Flushing Practices

Catheter materials vary widely, and this diversity plays a crucial role in determining the appropriate flushing protocols, including whether normal saline is suitable. Different materials exhibit unique characteristics such as versatility, surface texture, chemical compatibility, and susceptibility to encrustation or biofilm formation, all of which influence how they respond to flushing solutions. Understanding these distinctions empowers clinicians and caregivers to optimize catheter maintenance, prolong device life, and reduce complications.
Flexible materials such as silicone and polyurethane are commonly used in both short- and long-term catheters. Silicone’s smooth surface resists protein and bacterial adhesion better than some alternatives, making it less prone to blockage from biofilm buildup. This characteristic often means that flushing with normal saline alone can maintain patency effectively in many cases. However, polyurethane catheters, though similarly flexible, are somewhat more rigid and may have a higher propensity for clot formation; therefore, incorporating anticoagulant flushing (e.g., heparin) may be necessary, especially in long-term central venous catheters.
in contrast, latex catheters, while flexible and cost-effective, present unique challenges. Latex tends to provoke more tissue reaction and promote protein adsorption, increasing the risk of encrustation, especially in urinary catheters. Normal saline flushing might not be sufficient to prevent these deposits. For these catheters, specialized irrigation solutions with additives that break down mineral buildup or antimicrobial agents may offer better results in maintaining catheter function.
Material-Specific Flushing Considerations
| Catheter Material | Flushing Suitability with Normal Saline | Recommended Additional Measures |
|---|---|---|
| Silicone | Good for routine saline flushing due to smooth, nonreactive surface | Periodic heparin flushing if thrombotic risk is present |
| Polyurethane | saline suitable but may require heparin flushes in long-term use | Anticoagulants and monitoring for fibrin sheath formation |
| Latex | Saline flushing alone often insufficient to prevent encrustation | Use of acidifying or antimicrobial flushes recommended, especially for urinary catheters |
Moreover, the internal diameter and length of the catheter, often correlated with the material and design, influence the flushing force and flow dynamics. Catheters with narrow lumens require gentler flushing techniques to avoid damage, which can make the use of normal saline preferable, but also highlight the need for careful monitoring to detect blockages early. For instance, silicone tunneled central lines tend to have wider lumens suitable for routine saline flushes without high pressure, whereas smaller peripheral or specialty catheters may benefit from tailored flushing protocols.
Ultimately, understanding the interplay between catheter material and flushing solutions is essential. When managing catheters composed of more reactive or blockage-prone materials,normal saline flushing might need to be supplemented or replaced with alternative agents to maintain catheter integrity and patient safety.Tailoring flushing routines to the material specifics ensures that saline is used appropriately – neither underestimating the device’s vulnerabilities nor exposing it to unnecessarily harsh interventions.
Signs of Catheter Blockage and Flushing Interventions

Catheter blockage is a common and frequently enough preventable complication that can significantly affect patient comfort and treatment effectiveness. Recognizing the early signs of blockage is crucial to intervene promptly and avoid more serious outcomes such as infection, tissue damage, or interruption of essential medication delivery. Typical indicators that a catheter might potentially be blocked include a noticeable decrease in the amount of fluid draining compared to usual, the complete absence of fluid output for an extended period, or unusual symptoms like localized discomfort or swelling near the insertion site.
in patients with indwelling urinary catheters, for example, signs of obstruction often include bladder spasms, a sensation of urgency despite poor drainage, abdominal pain, or urine bypassing the catheter rather than flowing through it properly. In vascular access devices, resistance when flushing or an inability to aspirate blood are red flags signaling lumen occlusion or fibrin sheath formation. Awareness of these symptoms allows caregivers to act swiftly, reducing risks and improving catheter lifespan.
Flushing Interventions Using Normal Saline
Flushing with normal saline is a cornerstone intervention for clearing minor blockages caused by debris, sediment, or early clot formation within catheters.Saline’s isotonic properties help gently rinse the lumen without introducing harsh chemicals that might damage catheter material or irritate surrounding tissues. Routine flushing-following manufacturer and clinical protocols-can prevent buildup and maintain patency, especially for catheters made of silicone or polyurethane, which tolerate saline flushing well.
Though, it is indeed essential to apply flushing techniques correctly to avoid pushing blockages further or applying excessive pressure, which may damage the catheter or cause leaks. Use a gentle,steady push with a syringe of the appropriate size (usually 10 mL or larger) to create laminar flow and avoid shear stress. If resistance is met, do not force the saline; rather, consider alternative steps such as a pause-and-restoration approach or consulting clinical guidelines for additional flushing solutions like anticoagulants or specialized agents, depending on the catheter type and patient condition.
when Flushing Alone May Not Be Enough
While normal saline is effective for routine maintenance and minor occlusions, some blockages-particularly those involving encrustation with mineral deposits or biofilms-may require more specialized interventions. In urinary catheters made from latex or in long-term vascular catheters prone to thrombus formation, additional flushes incorporating agents such as heparin or acidifying solutions might be necessary to break down resistant deposits.Physical signs like persistent blockage despite flushing, increasing pain, swelling, or systemic symptoms such as fever warrant prompt clinical evaluation and potentially catheter replacement.
Practical reminders when intervening:
- Monitor urine output or catheter drainage frequently; a sudden change can be an early signal of blockage.
- Always follow aseptic technique to minimize infection risk during flushing.
- Document intervention details-volume of saline used, resistance felt, and patient symptoms-to guide ongoing care.
- If unsure about the cause or management of blockage, seek specialist advice rather than repeatedly flushing, which might worsen the problem.
By integrating vigilant observation with appropriately timed saline flushing and escalation protocols, caregivers can effectively maintain catheter function and greatly improve patient outcomes. For example, a patient with a silicone central venous catheter may experience smooth flushing with saline, illustrating how material compatibility supports the success of this approach, whereas a latex urinary catheter patient may need adjunct measures sooner to keep blockages at bay [[1]](https://mft.nhs.uk/app/uploads/2021/05/flushing-of-an-Indwelling-Catheter-and-Bladder-Washouts-Knowbots.pdf) [[3]](https://www.backtable.com/shows/urology/articles/how-to-flush-a-foley-catheter).
Expert Tips for Maintaining Catheter Patency With Saline

Maintaining catheter patency with normal saline is both an art and a science that hinges on attention to detail and adherence to best practices. One of the most effective ways to safeguard catheter function is to establish a consistent flushing schedule tailored to the catheter type and patient needs, as irregular or infrequent flushing can allow debris or biofilm to accumulate, leading to blockages.Using saline as an isotonic, tissue-amiable solution ensures the catheter lumen is gently cleaned without causing irritation or damage to the surrounding tissue, which is particularly important for long-term catheter care.
Applying the right technique during flushing significantly influences outcomes. Always use a syringe with an appropriate size-typically 10 mL or larger-to reduce excessive pressure that can damage the catheter wall or dislodge fragile thrombi that may cause embolism. Employ a slow,steady push to create laminar flow inside the catheter,which helps dislodge debris gently rather than forcing it and possibly worsening obstruction. If resistance arises, pausing and then attempting again can often prevent pushing blockages deeper and allows for safer management of partial occlusions.Frequent observation and documentation of catheter function are non-negotiable components of effective maintenance. This means carefully monitoring drainage volumes and any changes in patient symptoms to detect early signs of obstruction. For example, in urinary catheters, the sudden onset of bladder spasms or urine bypassing may indicate a developing blockage; in vascular catheters, difficulty aspirating blood or flushing resistance serve as red flags.Documenting the volume of saline used,presence of resistance,and patient response during each flush helps health professionals make informed decisions about whether to continue saline flushing or escalate care.
- Ensure strict aseptic technique: Preventing infection is paramount. Use sterile saline prepared according to clinical guidelines and sanitize hands and equipment before access.
- Use saline at room temperature: Cold solutions can cause vasospasms or discomfort, so warm saline slightly if needed.
- Choose catheter-compatible saline solutions: Avoid additives unless prescribed, as some solutions may be incompatible with certain catheter materials.
- don’t flush against resistance: Forcing saline under pressure can rupture catheters or injure vessel walls; rather, seek clinical advice or consider alternative agents cautiously.
Practical experience frequently enough reveals the importance of customizing flushing protocols. For instance, silicone or polyurethane catheters typically tolerate repeated saline flushes well and can be maintained purely with saline, while latex catheters or those prone to fibrin sheath formation might require adjunctive use of anticoagulants or specialized solutions as prescribed by clinicians. keeping open communication with patients about symptoms and signs of malfunction empowers earlier intervention and reduces complications.
By combining gentle flushing technique, vigilant monitoring, and strict infection control, caregivers can markedly extend catheter lifespan and enhance patient comfort. This proactive maintenance approach using normal saline not only prevents avoidable complications but also supports the effective delivery of therapy across diverse catheter types and clinical contexts.
Sterility and Infection Control During Catheter Flushing
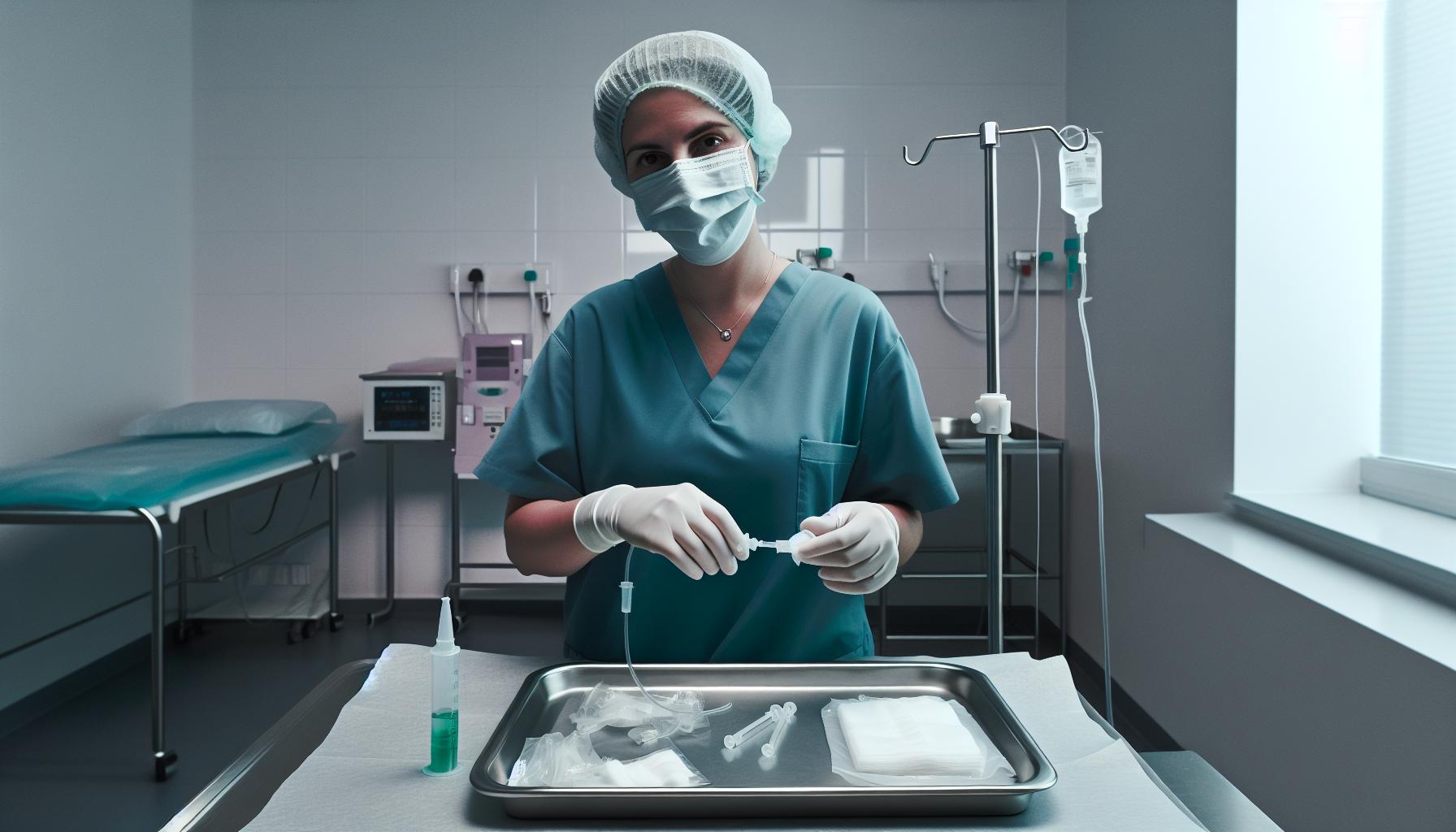
Maintaining impeccable sterility during catheter flushing is one of the most crucial defenses against potentially serious infections. Catheters provide direct access to sterile body compartments, making them a vulnerable point for microbial invasion. Even a minor lapse in technique can introduce pathogens that colonize the catheter surface or the adjacent tissues, leading to complications such as local infections, systemic bacteremia, or sepsis. Using normal saline as the flush solution is favorable as it is indeed isotonic and sterile when properly prepared, minimizing irritation and serving as a safe medium to clear potential debris without promoting microbial growth.
Strict adherence to aseptic technique begins with thorough hand hygiene and use of clean,preferably sterile,gloves before handling the catheter or flush equipment. The catheter access port, connection points, and syringe tips must never come in contact with non-sterile surfaces. It’s advisable to disinfect the catheter hub with appropriate antiseptics like chlorhexidine or alcohol wipes before insertion of the flushing syringe. Additionally, the saline used should be from a sterile commercial preparation or freshly made under controlled conditions to avoid contamination-improvised saline solutions without validated sterility pose significant risk. Storing saline in sealed containers and using it promptly after opening helps maintain its sterility.
- Prepare the flushing area carefully: Work in a clean, well-lit environment. Use sterile drapes if needed to protect surfaces.
- Use single-use syringes and avoid reusing flushing sets: Reusing equipment can introduce biofilm-forming bacteria onto the catheter.
- Avoid touching catheter tips, ports, or syringe needles directly: When connecting or disconnecting flushing devices, hold only the sterile parts.
- Control pressure during flushing: Besides mechanical concerns, excessive pressure can push microbes deeper into tissues or bloodstream.
One practical example from clinical settings involves urinary catheters, which are notorious for infection risk. Before flushing with saline, gathering all needed sterile materials and avoiding unnecessary breaks in the process decreases infection chances. Using a dedicated sterile basin to collect any drainage and discarding flush fluid immediately after use ensures contaminants are not spread back to the catheter or patient. In intensive care units or home care, protocols often mandate standardized training and competency assessments for caregivers performing catheter flushes, emphasizing sterility as a core component.
Recognizing and Preventing Contamination risks
Even with caution, contamination can occur due to environmental factors or human error. Staff should be vigilant for signs such as unusual catheter site redness,swelling,foul-smelling discharge,or fever,which could signal infection. if flushing resistance or blockage coincides with these signs, further microbiological evaluation and potentially more aggressive therapy may be warranted.
| Common Contamination Sources | Preventive Practices |
|---|---|
| Non-sterile hands or gloves | Rigorous hand hygiene; wear sterile gloves |
| Touching catheter ports/syringe tips | Disinfect ports before access; handle only sterile parts |
| Improper saline storage/preparation | use sterile,commercially prepared saline; store properly |
| Reusing syringes or flushing devices | Use single-use equipment for each flush |
| environmental contamination of work area | Clean workspace; use sterile drapes as needed |
demand disciplined technique and respect for infection transmission pathways. Combining the right preparation, the use of sterile normal saline, and constant vigilance can dramatically reduce the risk of catheter-related infections, ensuring that flushing fulfills its intended role of maintaining catheter patency without compromising patient safety.
recent Guidelines and evidence on Normal Saline Flushing

In recent years, the use of normal saline for catheter flushing has been reinforced by multiple authoritative bodies advocating for evidence-based protocols that balance efficacy with patient safety. One compelling development is the clear endorsement of normal saline as the preferred flushing solution because of its physiological compatibility and minimal risk profile. Clinicians widely recognize that saline’s isotonic nature prevents irritation and damage to catheter lumens and vascular or urinary tissues, unlike some anticoagulant or antimicrobial flushes which may carry additional risks or side effects.
Emerging research and clinical guidelines emphasize the importance of customizing flushing protocols depending on catheter type, patient condition, and clinical setting.As an example, in urinary catheter care, frequent irrigation with sterile normal saline is recommended to prevent obstruction from blood clots or debris, particularly in patients with hematuria. Protocols now frequently specify irrigation every four hours or as clinically indicated, using carefully prepared sterile saline-never tap water-to avoid infection [[2]](https://www.keckmedicine.org/wp-content/uploads/2022/02/Hematuria-Catheter-Irrigation-Procedure.pdf). Such data have prompted revisions in institutional policies to standardize not just the flush solution but also frequency and volume for different catheters.
Key Practical Points From Updated Protocols
- Use of commercially prepared or freshly made sterile saline: Ensures that the flushing fluid does not unintentionally introduce pathogens. Guidelines strongly discourage homemade solutions unless prepared under strictly controlled and verifiable aseptic conditions to maintain sterility [[3]](https://cinj.org/sites/cinj/files/documents/How-to-Make-Normal-Saline-for-catheter-Irrigation-2021.pdf).
- Flushing technique matters as much as the solution: newer recommendations highlight slow, gentle flushing to prevent damage to catheter materials and reduce the risk of forcing contaminants deeper into the bloodstream or surrounding tissues.
- Single-use syringes and equipment: Reinforced by recent infection control guidelines to minimize biofilm formation and cross-contamination, especially in outpatient or home care settings.
Healthcare systems worldwide are integrating digital resources, including video demonstrations like the one produced by swansea bay NHS, to enhance training and competency checks reflecting these guidelines [[1]](https://www.youtube.com/watch?v=mPbLhOcDvdE). This digital shift ensures caregivers at all levels can acquire real-time, practical skills for safe flushing under aseptic conditions, which is vital for reducing catheter-related infections and maintaining device functionality.
| Guideline Highlight | Clinical Implication |
|---|---|
| prefer sterile normal saline flushes over anticoagulant or antiseptic solutions | Reduces chemical irritation and risk of allergy or adverse reactions |
| Strict aseptic handling of flush solutions and devices | Minimizes infection risk through standardized infection control |
| Tailored flush intervals and volumes for catheter type and patient status | Prevents blockage and improves catheter longevity |
| Education and competency assessment for healthcare providers | Improves adherence to protocols and patient safety outcomes |
Ultimately, incorporating up-to-date evidence and guidelines supports both clinicians and caregivers in confidently choosing normal saline flushes when appropriate and performing the procedure to the highest safety standards. This ensures catheters remain functional with minimal complications, delivering better patient care and fewer costly interventions due to infection or obstruction.
FAQ
Q: How frequently enough should a catheter be flushed with normal saline to maintain patency?
A: A catheter should typically be flushed with normal saline every 8 to 12 hours or as per your healthcare provider’s instructions to maintain patency. Regular flushing prevents blockages and maintains catheter function. For detailed timing and technique, see the Expert Tips for maintaining Catheter Patency With Saline section in the article.Q: Can normal saline flushing help prevent catheter-related infections?
A: Flushing a catheter with sterile normal saline reduces the risk of infections by clearing residual medication and blood. However, maintaining strict sterility during flushing is essential. For infection control best practices, refer to the Sterility and Infection Control During Catheter Flushing section for more guidance.
Q: what should be done if resistance is felt when flushing a catheter with normal saline?
A: if resistance occurs during flushing, do not force the saline. this may indicate a blockage or catheter damage. Pause and consult clinical guidelines or a healthcare professional as outlined in Signs of Catheter Blockage and Flushing Interventions for safe troubleshooting steps.
Q: Are there any patient conditions that affect the use of normal saline for catheter flushing?
A: Yes, certain conditions like fluid restrictions or electrolyte imbalances may require alternative flushing solutions. Always assess patient-specific factors before flushing, as discussed in the When Not to Flush a Catheter With Normal Saline section for safe medical protocol adherence.
Q: Why is normal saline preferred over heparin solution for flushing some catheters?
A: Normal saline is preferred because it does not carry the bleeding risk associated with heparin. It effectively clears the catheter without anticoagulation, reducing complications.For a comprehensive comparison, review the Comparing Normal Saline to Other Flushing Solutions in the main article.
Q: how does the type of catheter affect the volume of normal saline used for flushing?
A: The catheter type determines the flushing volume; small-diameter catheters require less saline, typically 5-10 mL, while larger or multi-lumen catheters may need more. Follow the specific medical protocol outlined in the Medical Protocols for Flushing Different Types of Catheters section for best results.
Q: When is it inappropriate to flush a catheter with normal saline?
A: It is inappropriate to flush a catheter with normal saline if there are signs of infection, catheter damage, or occlusion that requires medical evaluation. Always follow the guidelines highlighted in When Not to Flush a Catheter With Normal Saline to avoid complications.
Q: How does improper flushing with normal saline impact catheter longevity?
A: Improper flushing can cause occlusions, increase infection risk, and reduce catheter lifespan. Consistent adherence to sterile technique and proper flushing protocols significantly enhances catheter durability, as emphasized in Common Mistakes to Avoid When Flushing Catheters.
For more detailed insights, consider reviewing the full article sections mentioned above, which provide comprehensive protocols and expert advice to optimize catheter flushing practices.
Closing Remarks
Understanding the proper protocol for flushing a catheter with normal saline is essential for maintaining catheter function and preventing complications.By following the recommended medical guidelines, you ensure safe and effective care that supports patient health and device longevity.if you’re looking to deepen your knowledge, explore our detailed article on catheter maintenance best practices or review the latest infection prevention tips to enhance your clinical skills.
Don’t hesitate to take the next step-whether it’s subscribing to our newsletter for ongoing updates, scheduling a consultation with one of our experts, or browsing our selection of trusted medical supplies designed for catheter care. If questions remain about flushing techniques or saline usage, we encourage you to leave a comment below or share your experience, helping build a community of informed healthcare professionals. Continually refining your approach to catheter protocols not only improves outcomes but also reinforces your confidence and authority in patient care.







